What is it?
Intrauterine insemination is a procedure, whereby processed sperm is placed into the uterine cavity.
Eugonia, as a certified IVF clinic with many years of experience in the field, can provide this fertility treatment among others, responsibly and always according to Greek legislation.
For further information about the procedure or if you want to book an appointment press here.
How is it performed?
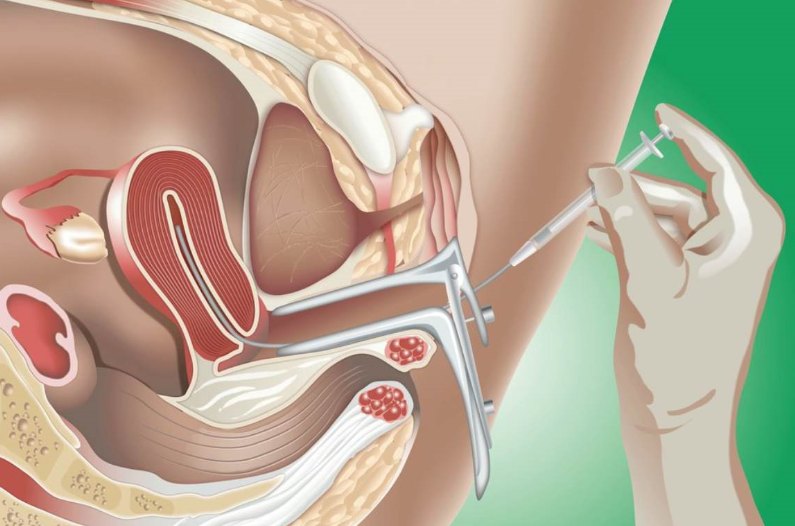
After sperm processing, spermatozoa are concentrated and activated, in a low volume (usually 0,5 – 1,0ml) of specialized culture medium. The washed sample is loaded into a thin, flexible catheter attached to an insulin syringe. A speculum is inserted into the vagina, to allow visualization of the cervix. The catheter is gently introduced through the cervix, into the uterine cavity, followed by injection of the processed semen sample. The catheter is then removed and the woman remains in a resting position for a few minutes. The whole procedure is painless and lasts for a few minutes, while after its completion the woman can return to her daily routine.
In which cases is IUI indicated?
IUI is indicated in:
- Young women with tubal patency
- Women with a “hostile” cervical mucus
- Women who do not have a regular cycle (i.e. polycystic ovary syndrome or ovulation irregularities); in such cases, ovulation is regulated with medication
- In cases with normal sperm quality or mild /medium sperm quality problems
- In cases of confirmed azoospermia, where donor sperm is used
- In single women, who want to use donor sperm
Is there any benefit from hysterosalpingography (HSG)?
As mentioned above, tubal patency is a prerequisite, with at least one of the two fallopian tubes being open. This can be tested via HSG, an X-ray that provides imaging of the uterus and fallopian tubes, and thus avoid an unsuccessful IUI due to fallopian tube blockage.
Does the IUI require the administration of drugs?
The IUI can take place in a natural cycle without medication or after single or multiple follicular development following drug administration. Usually ovarian stimulation is proposed to women with an unstable menstrual cycle, such as in polycystic ovarian syndrome cases.
How is the monitoring done?
Monitoring involves a series of ultrasound scans and blood hormone assessments. We believe that this combination allows for a better assessment than that provided by ultrasound monitoring alone. Ovulation may either occur naturally or it is induced 36 hours after hCG administration, when the follicle(s) have matured.
Which day of my menstrual cycle should the IUI take place?
Since the oocyte remains viable for only 24 hours following ovulation, we prefer to perform an IUI a few hours prior to or after ovulation.
What is the point in having an IUI if there are no sperm issues?
In some cases of unexplained infertility, IUI may be beneficial compared to unprotected sexual intercourse. The main difference is that the sperm is processed and activated in the laboratory, providing a final sample with spermatozoa with a better capacity to fertilize the oocyte, that are deposited straight into the uterine cavity.
When should sperm collection be done?
A few hours (usually 1-2 hours) before the scheduled IUI, the male partner must provide us with a semen sample. In cases of donor sperm, the sample is kept in our Cryopreservation Bank and thawed 1-2 hours before the IUI.
How many spermatozoa are required?
The lowest number of washed spermatozoa that gave a pregnancy, according to international bibliography, is 100.000. However, in order to have realistic chances of success, a minimum of 2.000.000 washed, motile spermatozoa is required.
What is the procedure for sperm preparation?
Processing of the semen sample involves density gradient centrifugation and culture media washing. As a result only actively motile spermatozoa are isolated from the semen. The latter includes white blood cells, immature genital cells and free oxygen species, which can cause DNA fragmentation and negatively affect the fertilization ability of the sample. With this procedure, sperm capacity may be improved and chances for fertilization are increased.
IUI success rates
IUI success rates depend on various factors (ovulation, female age, sperm quality etc.) It is considered that the average acceptable success rates range between 10 – 25% per treatment. This means that depending on the male partner's sperm quality, several attempts may be required before a pregnancy is established.
Age and IUI
If woman is over 40 years of age or if the levels of ovarian reserve are low (indicated by a decreased AMH), the success rates following an IUI are greatly reduced. In women of an older reproductive age, IVF is considered a more appropriate fertility treatment, as the chances of success are higher.
IUI or in vitro fertilization?
IUI is recommended in more “easy” cases of infertility. On the other hand, IVF is expected to yield higher success rates in the following cases:
- The quality of the sperm sample is significantly low
- The woman's age is over 40
- Low ovarian reserve
- Blocked fallopian tubes
- Multiple failed attempts with IUI
What you should be aware of after the IUI
If there is no discomfort following the procedure, there are no precautions you should take and you may return to your daily routine. You can also have sexual intercourse on the same day after the procedure, provided you feel no discomfort.
Modifications of the method
The main modification of IUI involves injecting a larger volume of fluid (5-6 ml instead of 1 ml that is usually used). The fluid containing washed spermatozoa is slowly released, filling the uterine cavity and the fallopian tubes, reaching the peritoneal cavity. Studies report slightly higher success rates compared to conventional IUI. There are however drawbacks: longer duration of the procedure and the use of a specific type of speculum that tightens the cervix, so that the fluid will not leak into the vagina.
Historical note
Intrauterine insemination is the oldest method of assisted reproduction. It was initially applied experimentally in animals in 1780 and in humans in 1791. It is a relatively simple method that requires placing sperm into the woman's vagina (vaginal), near the cervix (pericervical) or into the uterus (intrauterine). Intrauterine insemination is the only one of these methods applied today.